When a stroke strikes, time is measured in brain cells. Thousands of neurons can die every minute treatment is delayed — a reality that makes rapid response not just important but lifesaving. At Rice University, students are stepping into that urgency, working at the intersection of medicine, policy and communication.
In collaboration with the Houston Health Department, the Rice360 Institute for Global Health Technologies recently hosted a two-part Mobile Stroke Unit (MSU) Advocacy Hack-a-thon, inviting students to help solve one of the most pressing challenges facing this innovative technology: how to sustain it through public funding. The collaborative event was offered as part of Rice360’s new graduate certificate in global health technologies curriculum.
“This showed students that even when you have a technology that clearly works and improves lives, that doesn’t mean it will automatically be implemented,” said Kiara Lee, director of education strategy for Rice360. “They had to think about how to advocate for it — how to communicate its value and build the right support so that it reaches patients.”
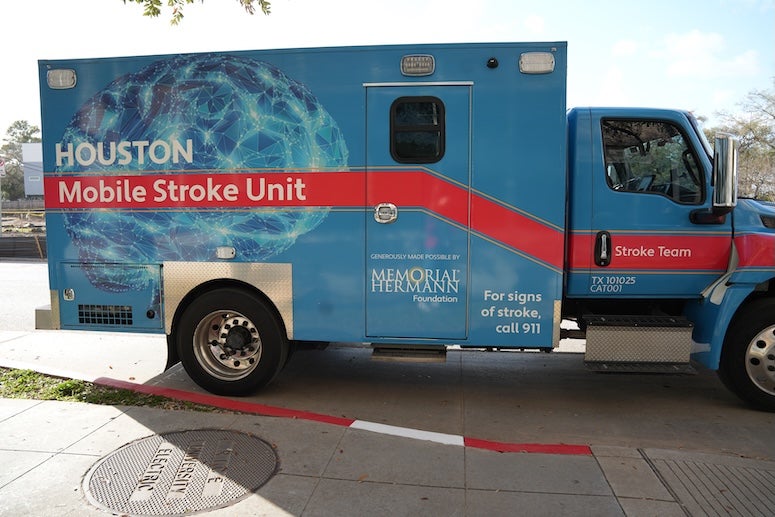
Houston is home to one of the world’s first MSUs — specialized ambulances equipped with CT scanners, telemedicine capabilities and clot-busting drugs that allow doctors to diagnose and treat strokes before a patient reaches the hospital. That timely care has been shown to significantly improve outcomes. Still, despite their success, MSUs face a major hurdle: They are reimbursed at rates similar to those for standard ambulances even though they function as mobile emergency rooms.

“Hard investigative work has shown that ultra early treatment of strokes can improve outcomes more than any other strategy,” said David Persse, chief medical officer for the city of Houston, who briefed students during the event. In his role with the city, Persse serves as the public health authority for the Houston Health Department, the EMS medical director for the Houston Fire Department and as a tactical physician for the Houston Police Department. “Mobile stroke units break through all the barriers to optimal care that have been assumed to be insurmountable before now,” he said. “Mobile stroke units may be the single greatest advancement in reducing disability in America in a decade or more.”
Despite their success, Persse noted that the systems in place don’t adequately support the infrastructure and operations needed to keep MSUs running. That gap between clinical impact and policy support became the hack-a-thon’s central challenge.
Held across two sessions March 5 and March 12 on the Rice campus, the event brought together students from across disciplines, including engineering, public health, policy, communications and medicine, to translate clinical evidence into persuasive tools for policymakers.
The first session featured expert briefings, including a deep dive into stroke care and MSU operations, followed by a live demonstration of the unit itself. Students then moved into brainstorming mode, working in teams to develop ideas with feedback from clinicians, researchers and city officials. By the second session, those ideas had evolved into polished deliverables: videos, infographics, policy briefs and advocacy pitch decks designed to make a compelling case for sustained funding.
“I wanted to provide the students with a real-world problem, hoping the policy pitch products they developed could be used in the solution and that they would learn from the experience,” said Loren Hopkins, professor in the practice of statistics at Rice and chief environmental science officer and bureau chief of the data science division for the Houston Health Department, who hatched the idea for the hack-a-thon. “I believe the students were inspired by the challenge and the urgency of the situation. The products they produced were remarkably different from each other and ranged from educational awareness videos for the public to shared revenue models. The judges felt each product could advance the cause in some capacity.”

For many students, the experience revealed a side of innovation they hadn’t fully considered.
“Those working on point-of-care devices often think, ‘Why wouldn’t you implement something that helps people at their doorstep?’” Lee said. “This helped them understand why — and what it actually takes to move something from idea to impact.”
The hack-a-thon emphasized three key areas: creating compelling media to humanize data, refining policy language and developing strategic advocacy approaches. Students also gained insight into the complexity of bringing medical innovations to scale — from regulatory hurdles and reimbursement structures to stakeholder coordination and public awareness.
“They learned that different people are required at different stages to effectively grow a product or program,” Lee said. “It reinforced the importance of building strong teams and seeking out specific expertise at different points along the product commercialization and implementation pipeline.”
The event is part of a broader, long-standing collaboration between Rice and the city of Houston, which has tackled public health challenges ranging from cardiac arrest response to air pollution and wastewater surveillance.
“Collaboration like this shows the power of bringing academia, community partners and local government together to solve real public health challenges, while also cultivating the next generation of public service leaders,” said Naomi Macias, assistant director at the Houston Health Department and a judge for the competition. “It’s important for us to leverage the talent and perspective of students — they bring fresh thinking, challenge assumptions and help us look at complex problems in new ways. The brilliant students at Rice University did exactly that, offering innovative ideas to help support and sustain the mobile stroke unit, while also gaining real-world experience that helps shape the next generation of public service leaders.”

While all teams presented solutions judges described as thoughtful and actionable, three stood out for their clarity, feasibility and potential real-world impact.
The first-place team earned top honors for a policy proposal that tackled one of the most fundamental barriers facing MSUs: reimbursement. The team’s solution called for Medicare to create a new, dedicated ambulance service level specifically for MSUs, effectively recognizing that these units function as far more than traditional ambulances. By proposing an eighth reimbursement category under existing federal regulations, the team outlined a pathway to cover the advanced capabilities onboard. Crucially, the students emphasized that this change could be achieved through a regulatory process led by the U.S. Department of Health and Human Services, avoiding the slower and more complex legislative route. Their proposal also addressed long-term cost implications, arguing that while upfront reimbursement would increase, earlier treatment could reduce hospital stays and downstream costs, ultimately benefiting the broader health care system.
The second-place team focused on aligning payment models with the realities of modern stroke care, framing its argument around a simple but powerful idea: The hospital is already reaching the patient — now the payment system needs to catch up. The team’s proposal introduced a pilot program built on an episode-based reimbursement model in which MSUs would receive standard emergency medical services payment plus a temporary add-on tied to patient outcomes over a 90-day period. The approach emphasized accountability with costs and recovery outcomes compared against traditional care pathways. If MSUs demonstrated better outcomes at lower overall cost, programs would share in the savings. Judges praised the model for building on existing Centers for Medicare & Medicaid Services frameworks while offering a pragmatic, testable path forward.
The third-place team took a more technological approach, proposing a comprehensive communications and decision-support platform known as StrokeLink. Designed as an AI-driven infrastructure system, StrokeLink aimed to optimize every stage of stroke response — from 911 dispatch to hospital handoff. The platform integrates predictive modeling to position units in high-need areas, real-time clinical decision support to assist treatment in the field and automated data-sharing tools to streamline transitions to emergency departments. It also incorporates features to address financial and language barriers, including eligibility screening for care coverage and multilingual patient communication tools. Judges noted that while more ambitious in scope, the proposal highlighted how advanced data systems could further enhance the effectiveness and reach of mobile stroke care.
“I was blown away when judging the seven teams at the recent MSU Hack-a-thon charged with figuring out a pathway to making MSUs financially sustainable,” said James C. Grotta, director of the MSU Consortium at UTHealth Houston and a judge for the event. “While they speed stroke treatment to the prehospital setting resulting in fewer patients with long-term disability, they are not currently reimbursed more than a routine ambulance. Some MSUs have had to sunset their programs due to the lack of reimbursement. Potential solutions ranged from targeting younger future patients and current caregivers with social media, raising philanthropic and federal grants to create MSU startup grants, having CMS redirect a portion of its downstream medical cost savings back to MSU programs, and addressing the messaging directly to CMS to change reimbursement pathways. I learned something new from each and every presentation.”
All the judges praised the ingenuity and real-world viability of the students’ solutions, noting that the ideas didn’t just diagnose problems but pointed toward actionable change.
“I love working with the students from Rice because they always come to a problem from an angle we hadn’t considered, often leading us to a much more creative and therefore more effective answer,” Persse said.