CONTACTS:
David Ruth Jade Boyd Katrina Burton
Rice University Rice University MD Anderson Cancer Center
National Media Director Science Editor External Communications
713-348-6327 713-348-6778 713-792-8034
druth@rice.edu jadeboyd@rice.edu kburton@mdanderson.org
Nearly 800,000 deaths prevented by declines in smoking
Feds tap Rice, MD Anderson experts for landmark study of tobacco policy and lung cancer
HOUSTON — (March 14, 2012) — U.S. tobacco-control programs and policies enacted after 1964 prevented more than 795,000 lung cancer deaths between 1975 and 2000, according to a landmark study by experts at Rice University, the University of Texas MD Anderson Cancer Center, the National Cancer Institute (NCI) and other institutions.
According to the study, if smoking in the U.S. had ceased following the release of the surgeon general’s first report on smoking and health in 1964, a total of 2.5 million people would have been spared from death due to lung cancer between 1975 and 2000. The results of the study were published online today in the Journal of the National Cancer Institute.
Lung cancer is the leading cancer killer for both men and women worldwide, and more than 80 percent of lung cancers are attributed to smoking.
Study co-author Marek Kimmel, professor of statistics at Rice, said, “It’s obvious that the less you smoke, the less likely you are to get lung cancer. The question has been: At what point do you start seeing the gains from reductions in smoking? What is the delay between changes in smoking behavior and reduction in deaths from lung cancer?”
Kimmel teamed with Olga Gorlova, associate professor of epidemiology at MD Anderson, and former Rice doctoral student Millennia Foy, now a postdoctoral researcher at the University of Texas Health Science Center at Houston, as part of the NCI-sponsored Cancer Intervention and Surveillance Modeling Network (CISNET). The network, which included the Rice-MD Anderson team and five teams across the world, used a comparative modeling approach in which they constructed detailed cigarette smoking histories for people born from 1890 through 1970, and then related the histories to lung cancer mortality in mathematical models. Using these models, the researchers were able to estimate the impact of changes in smoking patterns resulting from tobacco-control activities on lung cancer deaths from 1975 through 2000.
“While this many lives have been saved with existing tobacco-control initiatives, the overall health impact would have been much greater with more aggressive measures,” Gorlova said. “If we enhance these efforts, still more lung cancer deaths can be prevented. That’s what we hope will happen with the release of our findings.”
U.S. tobacco-control efforts since 1964 have included restrictions on smoking in public places, increases in cigarette excise taxes, limits on underage access to cigarettes and efforts to increase public awareness of the hazards of smoking.
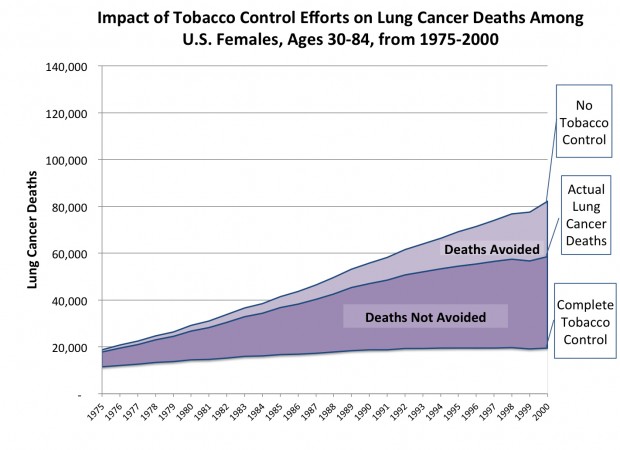
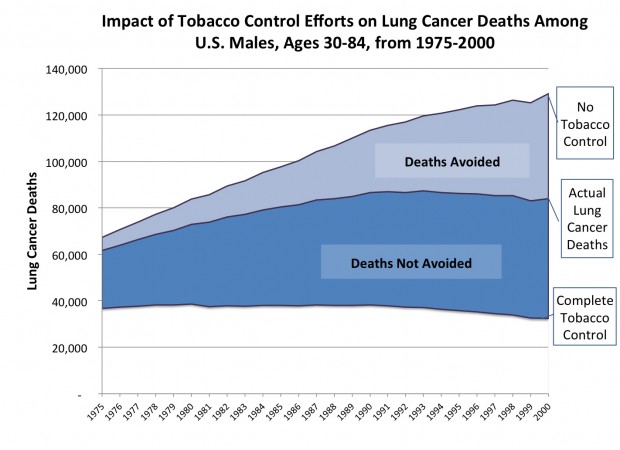
For the study, the researchers created three scenarios. In the first, called “actual tobacco control,” they used data on actual smoking behaviors of men and women in the United States. The second, called “no tobacco control,” predicted smoking behaviors that would have existed if no tobacco control policies had been put in place. In the third, called “complete tobacco control,” the researchers examined the possible outcome if all smoking in the United States had ceased as of 1965, the first full year after the surgeon general’s report on smoking and health was released.
The difference between lung cancer deaths in the “no tobacco control” scenario and the numbers of actual lung cancer deaths provided an estimate of the numbers of lung cancer deaths averted as a result of tobacco-control activities. This difference (graphically represented in two charts accompanying this release) was based on data from Yale University, which created one of the models used in the analysis. The researchers estimated that without tobacco-control programs and policies, an additional 552,000 men and 243,000 women would have died of lung cancer from 1975 through 2000.
Similarly, the difference between the “no tobacco control” scenario and the “complete tobacco control” scenario provides an estimate of the lung cancer deaths that could have been avoided if everyone who smoked quit in 1965 and no one started smoking. If tobacco-control efforts had been completely successful, an additional 1.7 million lung cancer deaths would have been averted from 1975 through 2000. In total, if all smoking had ceased completely in 1965, as many as 2.5 million fewer people would have died from lung cancer (1.6 million men and 883,000 women).
Nearly 800,000 deaths prevented by declines in smoking
“This is the first attempt to quantify the impact of changes in smoking behaviors on lung cancer mortality based on detailed reconstruction of cigarette smoking histories,” said lead author Suresh Moolgavkar of the Fred Hutchinson Cancer Research Center in Seattle. “The methods that were developed as a part of this research should prove to be invaluable to other researchers investigating the adverse health impacts of cigarette smoking.”
Kimmel and Gorlova said the methods developed by Rice and MD Anderson can be used to reproduce lung cancer patterns in any population, including patients enrolled in trials for new treatments and new screening technologies.
CISNET is a consortium of NCI-sponsored investigators who use statistical modeling to improve understanding of cancer-control interventions in prevention, screening and treatment. This modeling approach, which has been validated in several previous studies, can be used to guide public health research and priorities.
The other five CISNET centers that created models are Erasmus Medical Center in the Netherlands, Fred Hutchinson Cancer Research Center in Seattle, Massachusetts General Hospital-Harvard Medical School in Boston, the Pacific Institute for Research and Evaluation in Calverton, Md., and Yale University in New Haven, Conn.
-30-
High-resolution images are available for download at:
https://news2.rice.edu/files/2012/03/SMOKING-fem.jpg
CREDIT: National Cancer Institute
https://news2.rice.edu/files/2012/03/SMOKING-Male.jpg
CREDIT: National Cancer Institute
https://news2.rice.edu/files/2012/03/Marek_Kimmel.jpg
CAPTION: Marek Kimmel
CREDIT: Rice University
Located on a 300-acre forested campus in Houston, Rice University is consistently ranked among the nation’s top 20 universities by U.S. News & World Report. Rice has highly respected schools of Architecture, Business, Continuing Studies, Engineering, Humanities, Music, Natural Sciences and Social Sciences and is known for its “unconventional wisdom.” With 3,708 undergraduates and 2,374 graduate students, Rice’s undergraduate student-to-faculty ratio is 6-to-1. Its residential college system builds close-knit communities and lifelong friendships, just one reason why Rice has been ranked No. 1 for best quality of life multiple times by the Princeton Review and No. 4 for “best value” among private universities by Kiplinger’s Personal Finance. To read “What they’re saying about Rice,” go to www.rice.edu/nationalmedia/Rice.pdf.





Leave a Reply